Contents

Understanding the nervous system roots of PDA and practical ways to help your child.
If your child seems to avoid even the simplest requests—like brushing teeth or putting on shoes—and those refusals come with meltdowns, resistance, or full-blown panic, you might be dealing with something more than just defiance.

This blog will help you understand Pathological Demand Avoidance (PDA)—what it is, how it affects children, and the most effective approaches to Pathological Demand Avoidance treatment. You’ll learn how to support your child by calming their nervous system, building coping skills, and using brain-based strategies that foster lasting emotional and behavioral growth.
What is Pathological Demand Avoidance (PDA)?
Pathological Demand Avoidance (PDA) is a lesser-known but profoundly impactful behavior profile often linked to autism. Children with PDA experience an overwhelming, anxiety-driven need to avoid everyday demands—even ones they usually like. This avoidance isn't rooted in defiance or oppositional behavior; it's their brain's way of trying to stay safe and in control when they feel overwhelmed or powerless.
PDA was first identified by British psychologist Elizabeth Newson in the 1980s. While it isn’t officially recognized in the DSM-5, it’s widely acknowledged in the UK and by professionals specializing in neurodivergence.
Key Features of PDA:
- Extreme resistance to everyday demands
- Surface-level social skills but poor social understanding
- Mood swings and emotional outbursts
- Obsessive behavior, often focused on people
- Role-play or fantasy as a way to avoid demands
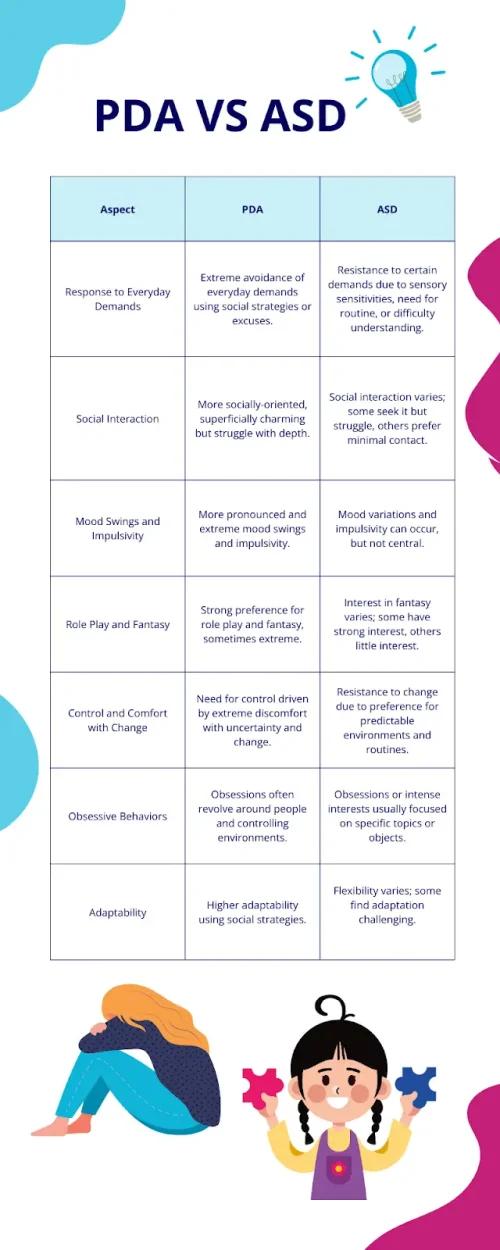
How is PDA Different from Autism or ODD?
While PDA is part of the autism spectrum, its presentation is often mistaken for Oppositional Defiant Disorder (ODD) or general behavioral problems because of the high level of demand avoidance and emotional outbursts. What sets PDA apart is that the resistance stems from intense anxiety, not a desire to disobey or assert power. This makes it especially easy for educators or providers unfamiliar with PDA to miss the signs and label the behavior as willful defiance.
PDA vs. Autism: PDA kids are often more socially engaged on the surface but lack true understanding.
PDA vs. ODD: PDA behavior is anxiety-driven, not intentionally rebellious. It’s not about saying “no” for control—it’s about avoiding demands to reduce panic.
Julia’s Story: Her 10-year-old son was labeled as defiant. He refused to follow instructions, argued constantly, and had intense meltdowns over what seemed like simple requests. But what looked like resistance was really panic from sensory overload, unpredictability in the classroom, and the constant feeling of being controlled. Once Julia discovered it was PDA driving his behavior—and not bad parenting or defiance—she shifted to low-demand parenting and co-regulation strategies. Everything began to change.
Comparison Table: PDA vs Autism vs ODD
FeaturePDAAutismODDMotivation Driven by anxiety and need for control Can vary; often overwhelmed by sensory or social input Willful defiance or opposition to authority Response to Demands Avoids demands through distraction, negotiation, or meltdown May comply or withdraw depending on sensory or social overload Often directly refuses, argues, or challenges rules Social Skills Surface sociability, but lacks depth in understanding Social communication difficulties; may appear aloof or awkward Often argumentative or hostile toward authority figures Common Triggers Any perceived loss of control or imposed task Sensory overload, social confusion, transitions Limits, rules, perceived unfairness Behavioral Strategies Low-demand parenting, co-regulation, flexibility Structure, sensory supports, behavioral therapies Consistency, behavior plans, clear rules Diagnosis Category Not in DSM-5; often diagnosed as part of ASD profile Autism Spectrum Disorder (DSM-5) Disruptive, Impulse-Control, and Conduct Disorders (DSM-5)
What Are the Signs of PDA in Children?
If you’ve ever wondered whether your child’s refusal to do simple things—like get dressed, transition to homework, or brush their teeth—is something more than just a phase, you’re not alone. PDA shows up in subtle but powerful ways, and recognizing the patterns is the first step toward helping your child thrive. Here's what to look for:?
Demand Avoidance Symptoms:
- Resist even routine tasks (e.g., brushing teeth, getting dressed)
- Use charm, distraction, or excuses to avoid demands
- Have meltdowns when pushed
- Prefer role play or fantasy to escape
- Seem sociable but struggle with real relationships
- Experience mood swings and anxiety when demands are placed

Common Mental Health Misdiagnoses that Overlap with PDA:
- ADHD
- ODD
- Anxiety disorders
Comparison Table: PDA in Girls vs PDA in Boys
FeaturePDA in GirlsPDA in BoysPresentation More likely to mask, internalize, and comply in public More likely to show externalized behaviors (meltdowns, refusal) Avoidance Tactics Uses social mimicry, withdrawal, or perfectionism Uses distraction, negotiation, or explosive outbursts Social Behavior Often overly helpful or people-pleasing as a masking strategy May appear oppositional or controlling with peers Common Misdiagnoses Anxiety, depression, eating disorders ODD, ADHD, conduct disorder Recognition & Diagnosis Often overlooked due to "quiet" or compliant appearance More likely to be flagged early due to disruptive behaviors
Girls with PDA are often missed or misdiagnosed because their distress may look like perfectionism, extreme people-pleasing, or withdrawal rather than aggression or defiance. It’s important to recognize these differences to ensure girls get the right support.
What’s Going On in the PDA Brain?
Children with PDA experience heightened threat sensitivity in the brain, particularly in areas that manage emotion, sensory input, and executive functioning. When a demand is placed—whether it’s a request to get dressed or start homework—their brain perceives it as a loss of autonomy, which triggers a fight-flight-freeze response.
Key characteristics of the PDA brain:
- Overactive amygdala: Triggers panic or shutdown over everyday tasks
- Impaired prefrontal cortex: Makes flexible thinking and transitions harder
- Chronic stress response: Keeps the nervous system in survival mode
That’s why traditional strategies don’t work—and why regulating the nervous system must come first. When the brain is calm, your child can think, learn, and respond more adaptively.
Why Does My Child Avoid Everyday Demands?
If your child suddenly shuts down, melts down, or pulls out every excuse in the book when asked to do something—even something they usually enjoy—you might be scratching your head wondering, "Why is this so hard for them?"
The truth is, the avoidance seen in PDA isn’t willful. It’s a nervous system reaction to a perceived loss of control. Their brain is on high alert, interpreting even everyday tasks like brushing teeth or putting on shoes as threats to their autonomy.
Understanding this is key: Your child isn’t trying to be difficult—they’re trying to stay safe.
What Demand Avoidance Looks Like:
- Meltdowns over transitions
- Avoiding eye contact or freezing
- Constant negotiation or refusal
Let’s be real: You’ve probably tried it all—charts, rewards, consequences—but nothing seems to stick. That’s because when your child’s nervous system is overwhelmed, even a simple request can feel threatening. Their brain reacts in panic—not defiance—leading to shutdowns, meltdowns, or total refusal.
Can You Have PDA Without Autism?
Some children with PDA traits don’t meet full autism criteria, but most professionals still consider PDA a profile within the autism spectrum because of the shared neurological and developmental characteristics.
While some clinicians disagree or hesitate due to its exclusion from diagnostic manuals like the DSM-5, research shows that the neurological underpinnings of PDA align closely with ASD, including heightened sensory sensitivities and difficulty with flexibility.
That said, PDA children often have a very different support need than those with classic autism presentations. Their demand avoidance is more intense, their anxiety more hidden behind social masking, and their behavior often misunderstood. This makes proper identification and support planning even more critical.
Expert Insight:
"PDA is not about oppositional behavior—it's about panic. These children need co-regulation, not compliance training."
— Dr. Ruth Fidler, UK PDA Researcher

How is PDA Diagnosed if It's Not in the DSM-5?
Even though PDA is not formally recognized as a separate diagnosis in the DSM-5 or ICD-10, many experienced clinicians in the U.S. acknowledge it as a valid and important profile, especially in the context of autism spectrum evaluations.
Instead of assigning a standalone diagnosis, a knowledgeable provider may document PDA traits as part of a broader diagnosis or note it as a descriptive profile:
- Autism Spectrum Disorder with a PDA profile
- Extreme demand avoidance traits linked to anxiety
Diagnostic Tools Often Used:
- Thorough parent interviews and developmental history
- Direct observation across multiple settings (home, school, clinic)
- Extreme Demand Avoidance Questionnaire (EDA-Q) or EDA-8
- Feedback from educators, therapists, or others familiar with the child
Important: Because PDA can mimic other conditions, many children are mistakenly diagnosed with ODD, ADHD, or generalized anxiety. That’s why it’s essential to seek out a PDA-informed professional or PDA psychologist—someone who understands that this is a nervous system issue, not a discipline problem.
Early recognition and the right language in an evaluation can make all the difference in getting appropriate support at home and in school. Understanding how to treat PDA autism begins with identifying it correctly and building a personalized plan based on nervous system regulation and connection.

How Do You Diagnose PDA
StageDescription Concern Identified Parent, teacher, or provider notices demand avoidance and emotional outbursts Initial Screening Developmental history and symptom checklists are reviewed Formal Evaluation Begins ASD assessments (e.g., ADOS-2, interviews, sensory profile) are conducted Demand Avoidance Recognized Clinician notes extreme avoidance, anxiety, and need for control Diagnostic Language Used Documented as ASD with PDA profile or extreme demand avoidance traits Support Plan Created Strategies include low-demand parenting, therapy, school accommodations
What Parenting Strategies Work for PDA Kids?
If you’re parenting a child with PDA, you’ve probably realized that traditional strategies—like sticker charts, time-outs, or consequences—only make things worse. That’s because PDA isn’t about being stubborn or disrespectful; it’s about anxiety and a deep need for control. To reach a PDA child, you need a completely different approach—one that prioritizes safety, collaboration, and emotional regulation.
Let’s calm the brain first. Then you can teach, guide, and support.
Effective vs. Ineffective Parenting Strategies for PDA
Ineffective StrategiesEffective Alternatives Direct demands ("Do it now!") Collaborative choices ("Would you like to do this or that?") Time-outs or punishments Co-regulation and emotional safety Sticker charts and reward systems Visual schedules and gentle scripts Demand Avoidance Recognized Clinician notes extreme avoidance, anxiety, and need for control Praise on demand Indirect praise and quiet encouragement
Low-Demand Parenting Works Best:
- Use collaborative language: "Would you like to do it now or after your snack?"
- Offer choices to create a sense of control
- Use written notes or visual cues instead of verbal demands
- Turn tasks into games or play when possible
- Praise indirectly to reduce pressure
PDA Parenting = Connection Before Correction.
Marcus, age 7, melted down over bedtime routines. Even the mention of brushing his teeth or turning off the TV would spark a screaming match or a complete shutdown. Once his mom shifted to using a visual bedtime schedule and playful choices ("Which PJs: sharks or ninjas?"), he began to feel more in control. They also built in a short movement break before starting the routine, which helped his body calm down. Within weeks, bedtime battles had softened into connection moments.

What Treatments Help Children with PDA?
There’s no one-size-fits-all approach when it comes to how to treat Pathological Demand Avoidance, but brain-based and anxiety-reducing strategies are key. If you're searching for PDA treatment autism or wondering about effective demand avoidance treatment, you're not alone—many parents are frustrated by a lack of clear answers. Fortunately, a combination of therapeutic support, parenting strategies, and lifestyle changes can lead to meaningful progress.
Effective Supports for Treating PDA Include:
- Neurofeedback (helps the brain regulate and reduces anxiety)
- Mindfulness & movement breaks
- Occupational therapy for sensory issues
- Therapy that focuses on co-regulation and flexibility
- Parent coaching to reduce escalation and reactivity patterns

Supplements That Support Regulation in PDA:
While there is no specific medication for Pathological Demand Avoidance, certain supplements may support brain function and emotional regulation. Always consult your provider before starting any regimen.
- Magnesium (especially L-threonate)
- Omega-3s
- Amino acids

How Can I Explain PDA to My Child and Others?
You don’t need to use clinical labels or overwhelm your child with complex explanations. But giving their experiences a name helps them feel seen and understood—and that’s the first step to co-regulating and building trust.
Say this: “Your brain likes to feel in control. That’s why some things feel really hard—even when you want to do them. It's not your fault—your brain is just trying to protect you.”
For Friends and Family:
- "My child isn’t misbehaving. Their brain is reacting to demands with panic."
- Provide gentle education and links to PDA resources
Will My Child Grow Out of PDA?
PDA isn’t something a child simply grows out of—but that doesn’t mean there isn’t hope for meaningful change and progress. What can and does happen is that children learn coping skills, self-awareness, and emotional regulation strategies that help them navigate demands more flexibly over time.
As their nervous system becomes more regulated—through therapeutic support, low-demand environments, and brain-based tools—those overwhelming reactions to everyday demands start to lessen. Your child can become more adaptable, confident, and in control of their responses.
The good news? With consistency, trust, and a calm, connected approach, your child can absolutely build the independence, resilience, and emotional strength they need to thrive in their own unique way.
Frequently Asked Questions About PDA
Is there a Pathological Demand Avoidance checklist?
Yes! You can download Dr. Roseann’s free PDA checklist to help identify common signs and support needs ➜ drroseann.com/pdachecklist
What is the best Pathological Demand Avoidance treatment for kids?
The best treatment is to regulate the nervous system and teach coping skills. A calm brain is the foundation for all learning and behavioral change.
What is the difference between PDA and ODD?
PDA is anxiety-driven and rooted in the nervous system. ODD is about willful defiance. PDA kids want to comply but can’t when they feel overwhelmed.
Can you have PDA without autism?
Most professionals agree PDA exists within the autism spectrum, but some children may have demand-avoidant traits without a formal ASD diagnosis.
Is PDA in the DSM-5?
No. PDA is not currently recognized as a standalone diagnosis in the DSM-5 used in the U.S.
What causes PDA?
It’s believed to be a combination of neurological, genetic, and environmental factors that influence nervous system development.
Is PDA treatable?
Yes. While it isn’t “curable,” PDA behaviors can improve dramatically with nervous system regulation, low-demand strategies, and targeted therapies.
What is the best Pathological Demand Avoidance treatment for adults?
While PDA in adults is less often recognized, the most effective treatment mirrors what helps children: regulate the nervous system and build flexible coping skills. This may include therapy with a PDA-informed psychologist, mindfulness practices, nervous system supports like neurofeedback, and accommodations in work or home life to reduce demand-based stress.
Final Thoughts on Treating PDA: Let’s Calm the Brain First
If you’ve been blamed, judged, or told to “just parent better,” let me say this:
You’re not doing anything wrong.
PDA isn’t about discipline or behavior charts—it’s a nervous system issue. That means the path to healing starts with regulation, not correction. Your child isn’t giving you a hard time… they’re having a hard time.
It takes time, patience, and consistency—but when we focus on calming the brain and teaching coping skills, everything starts to shift. Demands become less scary. Meltdowns become less frequent. And most importantly, your relationship with your child deepens.
💛 Want to take the first step? Download my free PDA Checklist to better understand your child’s behavior—and how to support them with compassion and clarity.

It’s gonna be OK.
Terminology
PDA: Pathological Demand Avoidance — a profile of autism where children strongly resist everyday demands due to anxiety.
Low-Demand Parenting: A strategy that reduces the number and intensity of demands placed on a child to lower anxiety and improve cooperation.
Neurofeedback: A non-invasive therapy that trains the brain to self-regulate using real-time feedback.
Surface Sociability: When a child appears socially adept but lacks deeper social understanding.
Citations
ReferencesDalkner, N., Unterrainer, H. F., Wood, G., Skliris, D., Holasek, S. J., Gruzelier, J. H., & Neuper, C. (2017). Short-term Beneficial Effects of 12 Sessions of Neurofeedback on Avoidant Personality Accentuation in the Treatment of Alcohol Use Disorder. Frontiers in Psychology, 8. https://doi.org/10.3389/fpsyg.2017.01688
Kildahl, A. N., Helverschou, S. B., Rysstad, A. L., Wigaard, E., Hellerud, J. M., Ludvigsen, L. B., & Howlin, P. (2021). Pathological demand avoidance in children and adolescents: A systematic review. Autism, 25(8), 136236132110343. https://doi.org/10.1177/13623613211034382
Malik, O., & Baird, G. (2018). Commentary: PDA - what’s in a name? Dimensions of difficulty in children reported to have an ASD and features of extreme/pathological demand avoidance: a commentary on O’Nions et al. (2017). Child and Adolescent Mental Health, 23(4), 387–388. https://doi.org/10.1111/camh.12273
Mathew, A. A., & Panonnummal, R. (2021). “Magnesium”-the master cation-as a drug—possibilities and evidences. BioMetals, 34(5), 955–986. https://doi.org/10.1007/s10534-021-00328-7
O’Nions, E., Christie, P., Gould, J., Viding, E., & Happé, F. (2013). Development of the “Extreme Demand Avoidance Questionnaire” (EDA-Q): preliminary observations on a trait measure for Pathological Demand Avoidance. Journal of Child Psychology and Psychiatry, 55(7), 758–768. https://doi.org/10.1111/jcpp.12149
Rylaarsdam, L., & Guemez-Gamboa, A. (2019). Genetic causes and modifiers of autism spectrum disorder. Frontiers in Cellular Neuroscience, 13(13). https://doi.org/10.3389/fncel.2019.00385Woods, R. (2020, August 5). PDA – a new type of disorder? Thepsychologist.bps.org.uk. https://openresearch.lsbu.ac.uk/item/8v10v
Dr. Roseann is a mental health expert in Neurodivergence who frequently is in the media:
- Helping Children Thrive Podcast Benefits of Neurofeedback for children with ADHD
- Very Well Mind What Is Asperger Syndrome?
- Parents Are Your Kid's Meltdowns a Sign of Rejection Sensitive Dysphoria?
Always remember... “Calm Brain, Happy Family™”
Disclaimer: This article is not intended to give health advice and it is recommended to consult with a physician before beginning any new wellness regime. *The effectiveness of diagnosis and treatment vary by patient and condition. Dr. Roseann Capanna-Hodge, LLC does not guarantee certain results.
© Roseann-Capanna-Hodge, LLC 2025

%20.png)















