
Does your child struggle with focusing, remembering, or are just not themselves? You might be dealing with something called Lyme Brain. It's more common than you think -- and it can seriously affect how your kid thinks, feels, and functions.
What is Lyme Disease?
While it may look like just tick bites and rashes, Lyme Disease can cause problems with memory, mood, and other brain functions and is also linked to illnesses like Autism, PANS/PANDAS, Arthritis and Multiple Sclerosis.

Lyme Disease is caused by a bacterium which gets into your child’s system through tick bites. Around 300,000 people are infected with Tick-Borne Disease annually (CDC) and is found in every continent except Antarctica with 14 US States having some of the highest concentrations globally.
How can Lyme Disease affect cognitive abilities and mental health?
- Cognitive Impairment and Brain Fog: Lyme disease can cause "Lyme Brain," with common problems like memory loss, focus problems, and slow thinking.
- Unexpected Mood Changes: Depression, anxiety, and irritability may come unexpectedly and your child might get completely overwhelmed.
- Executive Function Issues: Lyme disease messes with decision-making, time management, organizing tasks, and problem-solving. Your child may struggle with daily life functioning.
- Neurological Complications: Neurological Lyme disease can cause tingling or numbness in the limbs and brain fog.
- Chronic Fatigue and Sleep Disturbances: Constant tiredness and sleep problems like insomnia are common, making it harder for your child to function.
How do I manage neurocognitive effects?
- Following Medical Treatment Plan: Stick to prescribed treatment and antibiotics, if needed, for effective and faster recovery.
- Engaging in Cognitive Therapies: Engage in therapies designed to improve cognitive function.
- Adjusting to Healthy Lifestyle: Regular exercise combined with balanced diet and stress management techniques boost brain health.
Understanding Lyme's effect on your child’s brain is key to improving daily life. Make sure to seek medical support for proper care and guidance.
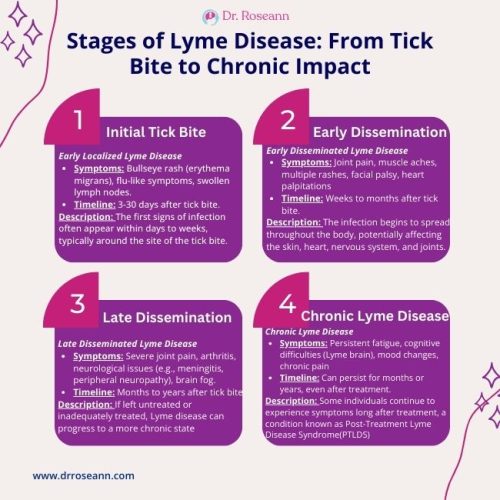
How Do You Diagnose Lyme & Tick-Borne Disease?
Lyme disease in children can trigger a wide range of physical, cognitive, and emotional symptoms.
Caused by the bacterium Borrelia burgdorferi, Lyme is most often spread by tick bites, though some believe other insects may also transmit it. It can even be passed from mother to baby during pregnancy—this is known as Congenital Lyme (Schlesinger et al., 1985).
Common challenges in diagnosing Lyme disease in kids:
- Symptoms may appear right after a tick bite or take months (even years) to show up.
- Many children never develop the classic bullseye rash—which appears in only 12% to 42% of cases.
- Kids may experience symptoms such as:
- Joint pain and fatigue
- Brain fog and memory issues
- Anxiety, mood swings, or confusion
- Misdiagnosis is common, especially with neurocognitive or psychiatric symptoms.
- Most traditional doctors lack specialized training in tick-borne illnesses, leading to delayed or missed diagnoses.
Functional MRI (fMRI) scans have shown how Lyme can disrupt brain function by affecting blood flow in areas tied to attention, memory, and emotional regulation. Early and accurate identification is key to helping children heal and function at their best.
How Do You Treat Lyme & Tick-Borne Disease?
Treating Lyme in children isn’t always straightforward. Here’s what you need to know:
- Get the right treatment A.S.A.P: Antibiotics can help during the early stages. But too often, kids are misdiagnosed or treatment is delayed because symptoms are missed.
- Get the right diagnosis: Standard Lyme tests can sometimes miss the mark—especially in children. A clinical diagnosis based on symptoms, history, and a physical exam can be just as important as lab testing.
- Avoid misleading criteria: While some providers still use the "5 out of 10 bands" as a benchmark for diagnosing Lyme on a Western blot test, it's important to know that fewer bands can still indicate infection.
- Trust clinical expertise: A thorough physical exam and listening to your child’s symptoms matter. Clinical judgment—not just lab results—can be the key to getting the right diagnosis and treatment.
https://youtu.be/mE6iqTlgJHI
Are There Other Kinds of Tick-Borne Diseases?
Yes. While many automatically think about Lyme Disease, they need to remember ticks carry multiple infections simultaneously. Symptoms of tick-borne diseases can include muscle aches, which appear with other flu-like symptoms.
Babesia is a tick-borne parasite infecting red blood cells and presents like malaria, with mild symptoms such as sweating. It can cause serious illness, especially when co-infected with Lyme disease, and is associated with neurocognitive and neuropsychiatric symptoms.
A teen patient struggled with severe anxiety for years, unable to leave her home. Despite showing clear signs of a tick-borne infection like Babesia, doctors overlooked it. During our first session, I was able to identify the proper diagnosis.
The QEEG brain map clearly showed the illness that the long list of physicians, psychiatrists, and psychologists had missed. That led to never being treated properly, She could then be referred to a Lyme physician for proper treatment.
Sadly, this teen had a clear-cut case of Lyme Disease and Tick-Borne Disease, but was never identified early and treated with antibiotics. This is an all too familiar story that leads to a case of Late-Disseminated Lyme, and more importantly, a lot of suffering and heartache.
What Neurocognitive & Neuropsychiatric Conditions Result from Lyme & Tick-Borne Disease?
Lyme disease can cause a wide range of neurocognitive and neuropsychiatric conditions, especially when not diagnosed or treated early. These may include:
- Brain fog and memory problems
- Attention issues and executive dysfunction
- Anxiety and panic attacks
- Depression and mood swings
- Obsessive-compulsive behaviors
- Irritability and emotional outbursts
- Sleep disturbances
- Sensory processing issues
- Psychosis or hallucinations (in rare cases)
Symptoms can show up early or long after the tick bite—especially if Lyme isn’t treated quickly. When the brain is affected, kids may struggle with focus, learning, or managing emotions. Many families see 5 to 7 doctors before getting answers (Bransfield, 2014), since these signs are often mistaken for mental health issues.
Research shows Lyme can impact the brain in big ways (Bransfield, 2007; Weintraub, 2009), and about 40% of patients develop nervous system problems (Fallon & Neilds, 1994). The good news? With the right treatment, kids can feel like themselves again.
What is Post Treatment Lyme Disease Syndrome (PTLDS)?
Even after treatment, some children still deal with lingering symptoms of Lyme disease. Post-Treatment Lyme Disease Syndrome (PTLDS) may cause fatigue, muscle pain, difficulty thinking or even mood swings.
Why PTLDS happens remains unclear but managing it requires a combination of regular doctor visits, symptom management, physical therapy and lifestyle changes. If symptoms persist, make sure to check in with a healthcare provider.
Is there A Connection Between Mental Health and Lyme & Tick-Borne Disease?
Lyme disease and other tick-borne illnesses often bring severe mental health challenges. Anxiety, depression, and cognitive issues often take hold leaving children struggling to function daily.
Research from Johns Hopkins University School of Medicine shows measurable brain changes in Lyme patients. It’s not all in their head but these issues are physical, coming from the impact of the disease to the brain.
Physical symptoms like fatigue, pain, and disrupted sleep can worsen mental health problems. Delayed diagnoses and inadequate treatment can also contribute to feeling isolated and confused.
A holistic treatment approach is needed to address both physical and mental symptoms. At our center, we use therapies like neurofeedback and PEMF to help ease the effects of Lyme disease.
What is Lyme & Tick-Borne Disease Prevention Important?
With Tick-Borne illness and Lyme Disease, prevention is key. Even if one already has Lyme Disease, they can get other tick-borne illnesses from another tick bite, so be sure to follow the BLAST protocol (lymeconnection.org).
The BLAST acronym:
- Bathe after outdoor activity
- Look for Ticks and rashes
- Apply repellent
- Spray the yard
- Treat pets
All five components are essential in preventing disease. Dr. Neeta Connally, a professor at WCSU and advisor for Lyme Connection, emphasizes that besides using repellant, taking a shower right after spending time outdoors can lower your risk of contracting the disease by 59%. Being mindful to avoid high tick areas and doing a tick check are also important steps.
What are Non-Invasive Treatments for Lyme & Tick-Borne Disease?
Diet, exercise and stress reduction are essential for healing Lyme and Tick-Borne Disease. The body is physiologically designed to deal with stress first and healing second, so practicing daily relaxation techniques needs to be part of one’s healing regimen.
In my office, we use a variety of brain-based techniques (Neurofeedback, Biofeedback, CALM PEMF™) to get the Central Nervous System (CNS) to calm down, which promotes self-healing.
Kids and families like yours have had significant improvements after taking our a safe and comprehensive approach to treating dysregulated brain symptoms in Lyme and PANS/PANDAS. In this program, we help families find calm and confidence again.
My best advice for you or your child is to find a Lyme and literate professional to work with so that you can get on the right path to healing.
Read more about: Causes, Symptoms, and Treatment for PANS/PANDAS
Parent Action Steps:
- Seek a Lyme Disease Specialist A.S.A.P
- Explore Brain-based Therapies
- Promote a Healthy Lifestyle at Home
- Take our FREE Solutions Matcher
Citations:
Bransfield, R. (2014). Neurocognitive and neuropsychiatric symptoms of tick-borne diseases: The challenges of diagnosis and management. Lyme Connection: Leir Center Presentation.
Bransfield R.C., Huismans B.-D., Phillips S., Scott J., Stricker R.(2007) Peer-Reviewed Evidence of Persistence of Lyme Disease Spirochete Borrelia burgdorferi and Tick-Borne Diseases
Dr. Roseann is a mental health expert in Neurodivergence who is frequently in the media:
- The Mack Talks Fighting the Stigma on Mental Health and Lyme Disease
- Living with Lyme (Podcast) Neurofeedback and biofeedback for PANS/PANDAS
- Learning to Slay the Beasts Podcast Treating PANDAS, PANS, and Lyme
Always remember… “Calm Brain, Happy Family™”
Disclaimer: This article is not intended to give health advice and it is recommended to consult with a physician before beginning any new wellness regime. *The effectiveness of diagnosis and treatment vary by patient and condition. Dr. Roseann Capanna-Hodge, LLC does not guarantee certain results.
Are you looking for SOLUTIONS for your struggling child or teen?
Dr. Roseann and her team are all about science-backed solutions, so you are in the right place!


%20.png)















